Period clots, the big jelly like pieces of endometrial lining that look like liver can be very disturbing. Add on period pain, cramps that make you wonder what you did in a past life to deserve this and heavy flooding, it can just feel like the proverbial kicking when you’re down.
If you are uncertain about period clots or not sure if yours are normal or something to worry about. You are not alone. Common questions I get from clients are:
- Are clots normal?
- Are they a sign of period problems?
- Do I need to speak to my doctor about clots?
- What can I do about my clots?
Are Period Clots Normal?
Period clots are common and can be indicative of a few underlying period problems. Small clots that are less than 1cm and that are not causing pain are fine. If you are getting larger clots and no other symptoms, then again, this isn’t anything to worry about.
However, if you are getting cramps or pain and other period symptoms, such as heavy periods, PMS and extreme bloating, then this can indicate something is going on.
What Are The Causes Of Period Clots?
There are two underlying issues here: firstly, lots of endometrial tissue, so lots of period blood, and secondly the blood having time to pool so that it can coagulate into larger pieces. The pain associated with clots alone is when they are large enough that the cervix has to open more to let them out, and cervix dilations are painful, think contractions in childbirth, or if you have had your cervix clamped in order to have an IUD inserted.
What Can Cause Heavy Periods?
There are a number of underlying causes here, hormonal imbalances such as oestrogen dominance, low progesterone and thyroid issues leading to heavy bleeding. You can take the period quiz to see if you have signs of any of these and get access to the videos that take you through what you can do about them.
Other times that hormones can be all over the place is during puberty and menopause. Again, taking a look at the quiz and videos can help somewhat with these changes, although there may be more specific needs for someone going through either of these life stages.
More serious causes of heavy periods can include endometriosis, in which endometrial like tissue that is sensitive to oestrogen grows in different places around the body. Usually people with endometriosis have period problems as well as the pain caused by endometriosis. There is also a condition called adenomyosis that is similar to endometriosis but instead refers to this tissue growing through the uterine wall.
These conditions do not just lead to painful periods, but extremely painful periods that painkillers do very little to touch, and can absolutely interfere with quality of life causing the need to withdraw and bed rest for several days a month. The only cure (and way to get a diagnosis) is laparoscopic surgery to remove the implants.

However, the symptoms can be greatly improved with diet and lifestyle for some people, and I have had clients in my clinic get their symptoms to a point where they are mild or negligible, so I know it is possible for some people. You can find out more about what you can do for endometriosis and adenomyosis here.
Fibroids are another condition that can cause heavy bleeding. Fibroids are polyps in the uterine tissue and can appear in any layer. Some can even be pedunculated or hang down too (which is one of the cases where womb and abdominal massage cannot be given for fibroids). Other symptoms of fibroids include heavy periods or painful periods, abdominal pain, lower back pain, a frequent need to urinate, constipation, pain or discomfort during intercourse.
If you think you have endometriosis or fibroids, please go to your doctor first for investigations and a diagnosis. Even if you choose to go for complementary treatments such as nutrition, lifestyle interventions and womb massage, the therapist will need to know if you do have a diagnosis and you will still need monitoring by your doctor to ensure that the conditions are being appropriately managed.
However, again with fibroids, symptoms can be greatly relieved with nutrition and lifestyle changes for some people.

What Can Cause Endometrium to Pool & Coagulate?
There are a few circumstances in which this happens as part of the reproductive life cycle. During puberty when the womb is expanding, after childbirth when it hasn’t yet returned to normal size and during menopause when the womb is shrinking back to the prepuberty size.
Some people will experience flooding due to the hormones and clots due to the hormonal fluctuations, and also observe an increase in clots due to the tissue behaving in different ways and endometrium collecting and pooling in various places.
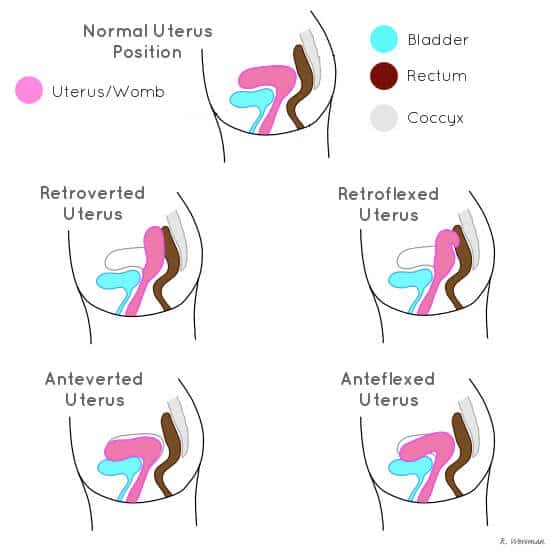
This is also possible when people have a backwards or forwards leaning womb, also known as retroflexed or retroverted uterus if it’s leaning backwards or anteflexed or anteverted uterus if leaning forwards.
The vagina should tilt backwards a little and the womb tilt forwards a little, nestled in between the bladder and rectum, and this position along with gravity and regular contractions of the uterine muscle help the period to exit the body.
If the womb is tipped far over, sometimes it can be bent in two so that thanks to gravity some of it leaves, and some of it pools in the top of the womb which is now bent so far over that it is upside down. This can cause a number of symptoms and also allow blood to collect and form clots. Womb massage is very helpful for this as is exercises that increases blood flow into the area such as walking, running, swimming and yoga.
Another reason for pooling can be if the womb is unable to contract properly. All muscle tissues are meant to contract in specific ways at specific times. If you are wondering what abnormal muscle contractions are, think about muscle cramps.
The womb is supposed to contract in certain ways too. If there are adhesions, glue like tissue either from conditions such as endometriosis, or from scarring or infections, these can cause pelvic congestion preventing the womb from being able to move and contract as it should.
Additionally, our sedentary lifestyles can result in mild constriction of blood flow to the womb, meaning slightly less oxygen and nutrients are getting to the muscle fibres. This can result in extra pain, cramps and not quite normal contractions. All of which can in some cases result in more clots.
Again, physical movement such as appropriate exercise, womb massage, or seeing a Womens Health Physiotherapist (UK) or Pelvic Health Physical Therapist (US) can help with this.

What You Can Do About Blood Clots Now?
If you think you may have endometriosis, fibroids or any underlying condition, please do go to your doctor to get checked out. You can take the period quiz to learn what underlying hormonal conditions could be going on, check out this blog post on heavy periods and this one on womb positions and more about womb massage.




