One question I’m regularly asked by my private clients is “my period is 22 days/56 days what can I do?”. You can pretty much insert any number of days into that question, it still won’t change my response which is: are you ovulating and when?
Ovulation is pretty awesome. Not only does it enable us to get pregnant (if we want to) but it helps with so many other important things, stabilising our mood after the drop in oestrogen, nourishing our thyroid, bone health, heart health and breast health.
But wait there is more. When you want to investigate period problems or fertility issues, maybe you think you have PCOS or endometriosis, you go to your doctor to get blood tests, scans and various other procedures to get a diagnosis. Whilst nothing can replace proper diagnostic testing, there are times when, you can’t get it done due to funding restrictions, insurance issues, you don’t have a great relationship with your doctor, you feel that a lot of these tests are intrusive.
But there is an easier way of finding the information you need too and it can help your doctor too. You can track when you ovulate. Not as in you have an app that tells you when you ovulate but you can learn the signs and symptoms that your body is preparing to ovulate right through to you have definitely ovulated. Isn’t that pretty awesome!
Why Tracking Ovulation Is Helpful For Period & Fertility Problems
There are several ways we can do this and several ways that you can do that I don’t recommend so much, but let’s take a look at them all and you can make up your own mind.
If you have regular bleeds but you are not ovulating, this is indicative or a number of issues, many of which can be helped, such as PCOS, hypothalamic amenorrhoea, stress amongst many other possibilities.
If you are ovulating but the time between ovulation and the start of your period is shorter than 12-14 days, we can start looking into other issues such as oestrogen dominance, high cortisol, low progesterone or thyroid issues.
These issues are also the causes of fertility issues (remember that your periods and fertility are the same thing), so if you are having issues trying to conceive it is really helpful to use this window to see what is going on.
Whilst I believe testing is great, it can be a bit misleading as different providers interpret ranges differently. Rather than pouring over test results, and trying to figure out optimal levels or even getting copies of your results, you can focus on is your body actually working the way you expect it too?
I find it amazing that we have this window to what our body is doing that means we don’t have to rely on so many external tests.

Charting Your Cervical Fluid
This is a great way to see that your body is preparing to ovulate.
How it works: when your follicles (eggs before they are eggs) are maturing in your ovaries, they start producing oestradiol, a type of oestrogen that is pretty awesome as it stimulates the growth of the uterine lining, and causing changes in the cervix to increase our fertility.
Oestradiol stimulates crypts in the cervical canal to start producing cervical mucus (I call it cervical fluid, CM or CF) which changes throughout the lead up to ovulation. First of all, it creates a plug in the cervix when we aren’t fertile in order to protect the womb from infection. As our oestradiol rises different types or cervical fluid are made that dissolve this plug resulting in a thick pasty or crumbly and opaque discharge.
As oestradiol rises further, the water content and structure of the cervical fluid changes further again, and does some pretty clever things: it filters out any defective sperm and nourishes the other sperm by changing the vaginal environment to a more alkaline pH. We will see our fluid become more liquid and clearer until we get stretchy clear egg white type cervical fluid which is our highly fertile fluid. It forms swimming lanes to literally propel sperm from even around the vaginal entrance (the labia) right up into the womb to get them on the way to the fallopian tube as an egg is about to be released.
Once an egg has released it only has 24 hours to be fertilised and when the body thinks it has done this, the cervical fluid will either suddenly stop or change to a thicker opaque fluid from an earlier phase. The last day of egg white cervical fluid is called the peak day. In most cases the peak day is considered to be the day you ovulated.
Pros: once you have taken instruction from a teacher and become proficient, you can read your body pretty well with nothing other than your ability to observe your cervical fluid which is pretty neat. It’s very cheap to use (free)! This method works really well when combined with basal body temperature tracking (BBT) in a symptom-thermal method.
Cons: this method takes a while to learn and because you can mis-interpret a lot, you must work with a qualified instructor. For this reason it is also expensive as it is something you need to get right first time. Many people do not realise that cervical fluid observations can be disturbed by a number of hormonal imbalances, medications, herbs, essential oils, inflammatory foods and alcohol.
If your body encounters stress, it will stop ovulation from occurring and then try again a few weeks later. You mistakenly identify the drop off in fluid to be your peak.
Methods that use this: Billing Ovulation Method (BOM), FEMM, Sympto-Thermal Method (STM) of Natural Family Planning (NFP), Sympto-Thermal Method of Fertility Awareness FAM).

Charting Your Cervical Changes
How this works: the oestradiol levels not only trigger the growth of your womb lining and cervical fluid it changes your cervix too!
When you are bleeding, your cervix opening, known as the OS, is closed. The cervix is low and hard. This is to let out the endometrium but we want to avoid infection going upwards. In preparation for ovulation, your cervical OS will open, the cervix will soften and rise, to allow for more comfortable penetration and to let sperm in.
Again, once ovulation has occurred the cervix will suddenly close, drop and harden. This is another peak showing that the body thinks it has ovulated.
Pros: again this is an easy method that relies on you knowing your body. There are less disturbances than with cervical fluid.
Cons: again this method is something you have to be taught. It is also unreliable on its own so it needs to be combined with another method such as cervical fluid or temperature charting or all together. Similar to cervical fluid, if exposed to sudden stress your cervix may revert back to an infertile pattern until your body is ready to ovulate again. Again it is a sign of your body preparing for ovulation but not confirmation of ovulation itself.
Methods that use this: either of the STM methods e.g. NFP and FAM in conjunction with other signs.

Charting Your Basal Body Temperature (BBT)
How this works: once you have ovulated, the empty follicle sac that burst to release the egg transforms into the corpus luteum and starts producing progesterone that raises the body temperature. Obviously various exercises, movement and activities will increase your body temperature, so this is only taken once a day first thing, immediately after three hours of sleep.
Once ovulation has occurred, and the corpus luteum has formed properly, there is a clear spike in BBT. In the methods that chart this, you learn to identify the base level of lower temperatures called the coverline and the qualifying temperatures above it.
Pros: you can confirm that your body has ovulated, and how long your luteal phase actually is.
Cons: it takes time to learn, to get into the habit and also things such as alcohol, medications, changing time zones, travel and disturbed sleep can affect your temperatures. It also takes time to learn and is learnt best with a qualified teacher.
Methods that use this: Basal Body Temperature (BBT), STM (both FAM and NFP).
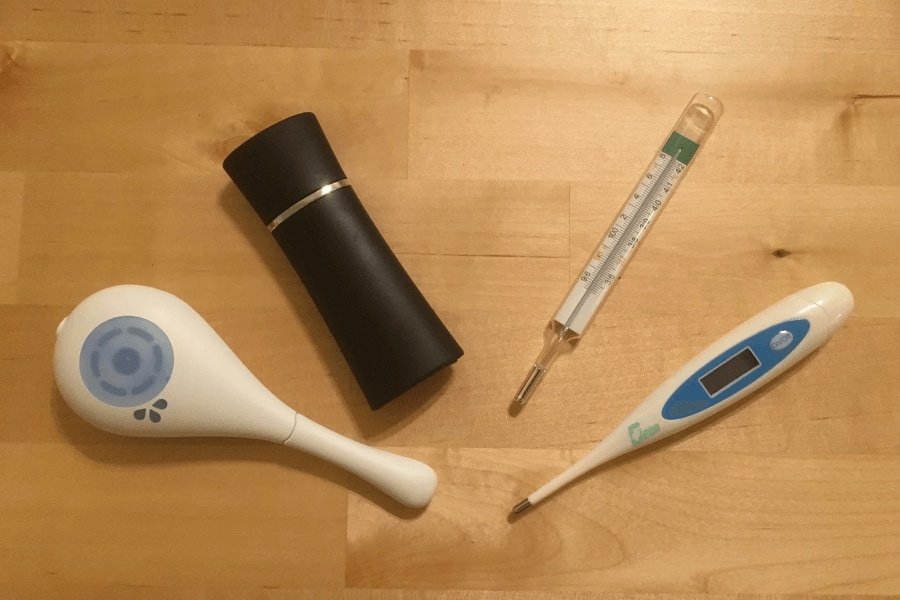
Symptom-Thermal Methods (STM) of Natural Family Planning (NFP) and Fertility Awareness (FAM)
These methods are very similar and there are some subtle differences between them but for now, we will consider them to be the same.
How this works: this is a combination of both the cervical fluid and the BBT methods so that you can see when your body is trying to ovulate and when it has ovulated. You can even add in cervix observations to this method as well as observations about your mood and feelings throughout the month.
Pros: this is the most comprehensive view of your body. Once you have gotten in to the swing of charting and understand all the nuances, you will understand so much about your body, it is highly addictive and most people tell everyone about how amazing their bodies are.
Cons: it requires, time and dedication to learn as well as an investment in a teacher or course as it is essential to learn from someone who is qualified. The same cons for all the above methods still apply, but because you are combining all these methods, you have the double check which helps confirm your findings.
Day 21 Progesterone Test
This is the famous progesterone test known as the day 21 test.
How this works: this test is taken 7 days after you ovulate and it measures your progesterone levels. Your doctor can order this.
Pros: this is a great test of accurately measuring progesterone levels and it is very useful to get done.
Cons: most women (and often medical professionals) do not know when you ovulate so they don’t know when 7 days post ovulation would be. Instead they assume that your cycle is 28 days and that you ovulated on day 14, therefore day 21 is 7 days post ovulation. However, if you ovulated earlier, or later than that, you are not getting a true reading of progesterone 7 days past ovulation. (The above methods can help you to identify when you should be doing the test).
Ultrasound Scans
This is highly useful as it shows follicle size in the lead up to ovulation and has a characteristic “ring of fire” on the ultrasound once it has turned into a corpus luteum.
How this works: a trans-vaginal ultrasound with a radiographer is performed to show the ovaries, follicles and corpus luteum (and potentially a pregnancy later on).
Pros: this is a very accurate method and you can see what is going on in the ovary.
Cons: not everyone has an ultrasound machine and radiographer handy or can afford to get one done every month to see if they are ovulating. It is not clear whether there is any long term health issues with people who are regularly exposed to ultrasound and more research needs to be done in this area.
Endometrial Biopsy
One of the functions of progesterone is to mature the womb lining (endometrium) and this can be examined by removing some of the lining and examining it. An endometrial biopsy is used to determine if a woman has ovulated, and if the endometrium has been affected by progesterone.
How this works: During this office procedure, a small amount of endometrial tissue from inside the womb is removed and examined under a microscope. This needs to be done just before menstruation is expected to begin. The physician will need to know the day that your period starts after the biopsy so that they can correctly interpret the sample.
Pros: This is fairly accurate and a skilled physician will be able to make a number of useful observations from this procedure.
Cons: charting BBT or using an OPK (see below) is also needed to help identify the time to do this procedure. This is an invasive procedure with more risk, cost and not necessarily easy to access. This would be more suitable for someone undergoing fertility investigations who needs that level of information available.
Ovulation Predictor Kits (OPKs)
These are the famous pee sticks!
How this works: to trigger ovulation, our pituitary sends a surge of two hormones, lutenising hormone (LH) and follicle stimulating hormone (FSH). This test detects the surge in lutenising hormone in the urine to let you know your body is trying to trigger ovulation.
Pros: easily available and can be gotten cheaply. Relatively easy to use. You can also use them to confirm pregnancy in some situations.
Cons: they can be expensive, and sometimes difficult to interpret. Cheaper kits are notoriously unreliable and they do not confirm that ovulation occurred, only that it happened. Unfortunately some ladies with hormonal disturbances such as PCOS with have raised LH so this test is not useful to them at all.
Ovulation Predictor Apps
This are those apps that you enter in some information and they tell you when you are fertile or when you have ovulated.
How this works: in many cases these are working on one of several calculations, I have used a number that use different ones and I have to say they are often wrong.
Pros: they take a lot of the brain work out of trying to track ovulation.
Cons: I have yet to see one that is consistently accurate, and these apps, if free often sell on your data and everything you put in to the app to other companies and in one case, the company was selling the data including social security numbers and intercourse timings to the US government. I have also had some of these companies offer to sell me data of their users. Note that any data driven services that is free, you are usually the product. Please check out the privacy policy and ensure that you are happy with it before signing up to any cycle charting app.
What I Recommend
I am biased as I am a long term user and teacher of the sympto-thermal methods because they tell me so much about my body and my clients without having to pour over test results and test ranges.
You can learn the how to start charting with the sympto-thermal method in my intro course here.
You can also sign up to my free cycle charting toolkit which explains the menstrual cycle in more detail, and takes you through charting your emotions, and cervical fluid observations at the top of the page.




